Posted by: Ophthalmology Associates of the Valley in Eye Health

Ozempic. Wegovy. Mounjaro.
These names have become nearly impossible to avoid, showing up in waiting rooms, on social media, and in conversations between patients and their doctors.
GLP-1 receptor agonists have reshaped how medicine approaches both type 2 diabetes and obesity, and their use continues to climb. As millions of people begin or continue GLP-1 therapy, a critical question has emerged in ophthalmology: what are these drugs doing to the eyes?
The answer, as new research makes clear, is complex.
How GLP-1 Medications Work

GLP-1 agonists mimic a naturally occurring hormone called glucagon-like peptide-1, which plays a role in regulating blood sugar after eating.
When stimulated, GLP-1 signals the pancreas to release insulin, slows how quickly the stomach empties, and reduces appetite, a combination that makes these medications effective for both blood sugar management and weight loss. The most widely prescribed include semaglutide (Ozempic, Wegovy) and tirzepatide (Mounjaro, Zepbound).
Because these medications affect metabolic processes throughout the body, changes to blood sugar levels, fluid balance, and blood flow can reach far beyond the digestive system. The eyes, with their intricate network of blood vessels and pressure-sensitive structures, are no exception.
The Retinal Risk That Concerns Eye Doctors Most
One of the more counterintuitive findings in GLP-1 research involves diabetic retinopathy. When blood sugar has been elevated for years, the blood vessels in the retina become fragile and vulnerable. The instinct might be to assume that rapidly lowering blood sugar would be protective, but the biology doesn’t always work that way.
When glucose levels drop quickly, those already-damaged vessels can experience added stress, leading to early worsening of existing retinal disease. This phenomenon has been observed with several effective diabetes treatments, not just GLP-1s.
For patients who already have diabetic retinopathy or who have struggled with blood sugar control over many years, this is particularly relevant. The risks are concentrated in patients with pre-existing retinal vulnerability, and, in the long run, better glucose control typically leads to healthier retinal outcomes. But the transition period matters, and close monitoring during early GLP-1 therapy is important.
NAION, A Rare but Serious Optic Nerve Risk

One of the most discussed ocular concerns linked to GLP-1 therapy is non-arteritic anterior ischemic optic neuropathy, or NAION, sometimes described as an “eye stroke.”
NAION occurs when blood flow to the optic nerve is suddenly reduced, causing painless but often permanent vision loss in one eye. Unlike many eye conditions that develop gradually, NAION can appear overnight. Many patients notice it when they wake up.
Researchers believe the mechanism may involve rapid drops in blood sugar, disrupting blood flow to the optic nerve, though this is not yet fully confirmed. For patients with a naturally small cup-to-disc ratio, a structural characteristic of the optic nerve, the risk appears higher. Other factors such as hypertension, high cholesterol, and obstructive sleep apnea also elevate individual risk.
Several of these are the same conditions that often prompt a prescription for GLP-1 therapy in the first place.
The overall risk of NAION remains low, and for most patients, the cardiovascular and metabolic benefits of these medications continue to outweigh the risk. But it is a risk worth knowing about before starting treatment, particularly for patients with pre-existing retina or optic nerve conditions.
Who Faces the Highest Risk
Not every patient starting a GLP-1 medication carries equal ocular risk. Certain profiles warrant more careful monitoring:
- Patients with existing diabetic retinopathy, particularly those with a history of poor blood sugar control
- Patients who have been diagnosed with or are at risk for age-related macular degeneration
- Those with hypertension, high cholesterol, or obstructive sleep apnea
- Patients with a small cup-to-disc ratio, which can only be assessed during a dilated eye exam
- Those starting semaglutide specifically, given its stronger association with both NAION and diabetic retinopathy compared to tirzepatide
Knowing your individual risk profile before starting therapy, not after a vision change occurs, is the most effective approach.
What Patients Can Do Before and During GLP-1 Treatment
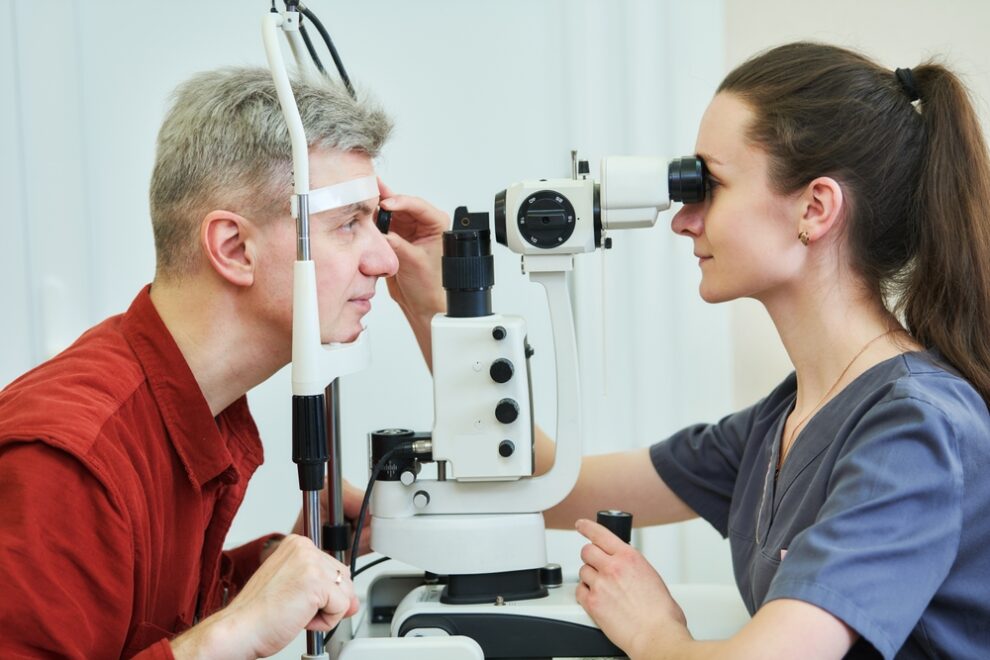
The American Academy of Ophthalmology recommends that anyone beginning GLP-1 therapy, especially patients with diabetes or a history of AMD, have a comprehensive dilated eye exam either within the 12 months before starting treatment or within one month of beginning therapy.
This baseline exam documents the current state of the retina and optic nerve, making it far easier to detect any meaningful changes that arise later.
During treatment, patients should not wait for a scheduled appointment if something changes. Sudden, painless vision loss in one eye, blurred or distorted central vision, or any new visual symptom that appears quickly is a reason to call an eye doctor right away, not to wait and see. NAION in particular moves fast, and early evaluation matters.
The research on GLP-1 medications and vision is still developing. Clinical trials specifically examining the effects on diabetic eye disease are currently underway, and their results will sharpen what is currently a picture of mixed signals.
For now, what is clear is that anyone taking or considering these medications deserves a thorough eye evaluation as part of their overall health plan.
Are you starting or currently taking a GLP-1 medication and want to make sure your vision is protected? Schedule an appointment at Ophthalmology Associates of the Valley in Encino and West Hills, CA.

